Sinus Headaches and Allergic Rhinitis
I came to Doctor Devi a year ago with sinus headaches, shortness of breath, coughing, runny nose and wheezing. Within the first two months, my sinus headaches were reduced by almost 90 percent. The coughing and wheezing are virtually all gone. Now, we are working on eliminating allergy symptoms. I have been very pleased with her treatment and I have recommended her to many others.
Jim Ashley
Anaheim, CA
Study: Incidence of nasal allergies set to go up in UAE
Survey reveals condition affects patients’ productivity

(Source: Gulf News, Published: March 15, 2012, By Janice Ponce De Leon, Staff Report)
Dubai: Regular sneezing, runny nose, nasal congestion, itchy eyes, cough, and headaches — these are just symptoms of allergic rhinitis which affects one in three adults in the UAE.
But beyond these symptoms lie burdens patients carry, and the numbers of affected people are projected to increase, doctors have warned.
Around the world, an estimated 400 million people are affected by this disease. And by 2020, a recent study predicted that one in two people up to 14 years of age worldwide may be affected.
What is Rhinitis?
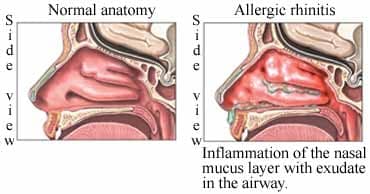
The term “rhinitis” is used to describe nasal inflammation that results in rhinorrhea (colloquially known as “runny nose”), congestion, nasal itch, sneezing, postnasal drainage, and in some patients, ocular symptoms such as watering eyes. It represents one of the most frequently encountered chronic conditions for which medical care is sought.
Rhinitis Types
Allergic rhinitis
Allergic rhinitis takes two different forms seasonal and perennial. Symptoms of seasonal allergic rhinitis occur in spring, summer, and/or early fall and are usually caused by allergic sensitivity to pollen from trees, grasses or weeds, or to airborne mold spores.
Other people experience symptoms year-round, a condition called “perennial allergic rhinitis.” It’s generally caused by sensitivity to house dust, house dust mites, animal dander, and/or mold spores. Underlying or hidden food allergies are considered a possible cause of perennial nasal symptoms.
Some people may experience both types of rhinitis, with perennial symptoms worsening during specific pollen seasons. As will be discussed later, there are also other causes of rhinitis.
Types of allergic rhinitis
- Allergic rhinitis may occur only occasionally, after contact with allergens from food or animal hair.
- Allergic rhinitis that always occurs at a certain time of the year, as a result of reactions to the pollen of trees, grasses or weeds, is called seasonal rhinitis.
- If allergic rhinitis occurs throughout the year, it is called non-seasonal, and it is most likely caused by house dust and dust mites.
Common hay fever symptoms include:
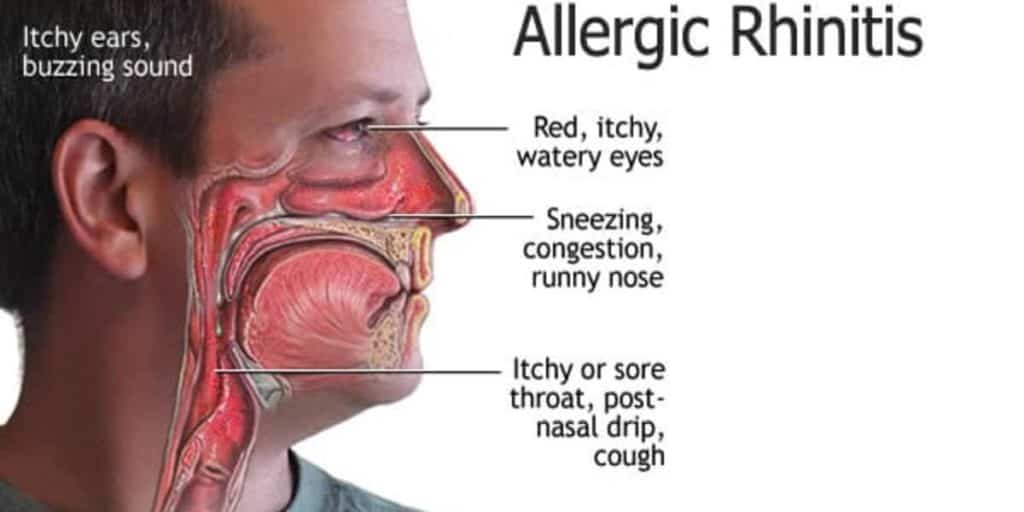
- You sneeze again and again, especially after you wake up in the morning.
- You have a runny nose and postnasal drip. The drainage from a runny nose caused by allergies is usually clear and thin. But it may become thicker and cloudy or yellowish if you get a nasal or sinus infection.
- Your eyes are red, watery, and itchy.
- Your ears, nose, and throat are itchy.
Is allergic rhinitis ever the cause of other problems?
Some known complications include ear infections, sinusitis, recurrent sore throats, cough, headache, fatigue, irritability, altered sleep patterns, and poor school performance.
Occasionally, children may develop altered facial growth and orthodontic problems. Allergy treatment can eliminate or alleviate most of these problems.
Medical Treatment for Hay Fever
There is a vast array of over-the-counter and prescription medications for treating hay fever symptoms. Some patients may find that a combination of two or three medications works much better than just one.
It is important for parents to remember that some hay fever medications are just for adults. If you are not sure, talk to a qualified pharmacist, or ask your doctor.
Medications include:
Antihistamine sprays or tablets
These are commonly available over the counter. The medication stops the release of the chemical histamine. They usually effectively relieve symptoms of runny nose, itching, and sneezing. However, if your nose is blocked they don’t work. Newer antihistamines are less likely to cause drowsiness than older ones – but older ones are just as effective.
Eye Drops
These reduce itching and swelling in the eyes and are usually used alongside other medications. Eye drops containing cromoglycate are commonly used.
Nasal Corticosteroids
These sprays treat the inflammation caused by hay fever and are safe and very effective long-term treatment. Most patients may have to wait about a week before experiencing any significant benefits. Some patients may notice an unpleasant smell or taste and have nose irritation.
Oral corticosteroids
For very severe hay fever symptoms the doctor may prescribe prednisone in pill form. They should be prescribed only for short-term use, because of their long-term link to cataracts, muscle weakness, and osteoporosis.
Another medical treatment is Immunotherapy (allergy shots) which is a proven treatment approach providing long-term relief for many people suffering from allergic rhinitis. It works by gradually desensitizing the patient’s immune system to the allergens that trigger their symptoms.
If your allergies bother you a lot and you cannot avoid the things you are allergic to, immunotherapy may help prevent or reduce your symptoms. To have this treatment, you first need to know what you are allergic to. However, immunotherapy can potentially lead to lasting remission of allergy symptoms, and it may play a preventive role in the development of asthma and new allergies.
One of the best things you can do is to avoid the things that cause your allergies. You may need to clean your house often to get rid of dust, animal dander, or molds. Or you may need to stay indoors when pollen counts are high.
“Decongestant nasal sprays should be avoided, especially in the long term, as they can cause rebound congestion and reduced efficacy over repeated use. Anti-histamines (to treat allergy) can be used, but one has to be aware of their potential side effects like drowsiness, weight gain and, in rare cases, heart arrhythmias (irregular heartbeat),” – Dr. Michael Loubser.
How can we help ourselves?
Allergic rhinitis is not a serious and difficult disease, but it significantly affects the quality of life and can cause a number of other problems: fatigue, irritability, difficulty in social relationships. You can help yourself by avoiding allergens.
- In case of pollen allergy, one should follow “allergic prognosis”, in the case of high concentration of pollen our advice is to reduce going out (morning, evening), close the windows, and ventilate the room in the afternoon. Face masks do not help, because they become wet so that pollen particles stick to them.
- In case of allergies to dust mites or house dust one should remove carpets and other “collectors” of dust, reduce the humidity in the rooms where you are staying, use antiallergenic bedding, and maintain it with special detergents and dry it quickly. There are very powerful vacuums with special filters that prevent the return of allergens into the air.
- In case of allergy to animal hair, unfortunately, one should avoid being near animals. It is believed that the allergens are actually in their saliva, which is specially retained on the hair.
- In case of allergy to mold, one should reduce the humidity in the rooms where you are staying, remove indoor plants, thoroughly clean the bathroom and other damp rooms.
- In the case of food allergies one should check the content of the food that is eaten, and also the declaration of the product since larger amounts of preservatives and colors also cause allergic reactions.
Non-allergic rhinitis
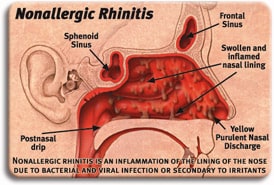
Non-allergic rhinitis is an extremely frustrating sinonasal disorder that is characterized by all the same symptoms of sinusitis and allergies, but NOT due to sinusitis or allergies. Rather, I consider non-allergic rhinitis to be the over-sensitive nose syndrome whereby breathing in air containing particulates (whether smoke, perfume, dust, pollen, etc) PHYSICALLY irritates the nose causing symptoms.
Symptoms of non-allergic rhinitis can include:
- A blocked nose
- A runny nose – this may be through the nostrils or down the back of the nose (catarrh)
- Sneezing – although this is generally less severe than in allergic rhinitis
- Mild irritation or discomfort in and around your nose
- Reduced sense of smell
Possible causes of non-allergic rhinitis include:
- Environmental irritants. Particulate pollutants, dust, smog, secondhand smoke, chemical fumes, can all cause rhinitis without true allergies. In children, one of the most common sources of environmental irritants that I have found in my clinics is the chlorinated pool.
- Hormonal changes. Women and especially pregnant women can experience non-allergic rhinitis as a result of hormonal changes.
- Infections. A common cause of nonallergic rhinitis is a viral infection – a cold or the flu. This should clear up within 2 weeks. Infectious rhinitis can become chronic, and usually includes a sinus infection – chronic rhinosinusitis.
- Foods and drinks. Some foods can cause rhinitis and swelling of the nasal membranes – with resulting nasal congestion – without true allergies.
- Medications. Some medications can cause nonallergic rhinitis. Examples include the non-steroidal anti-inflammatory drugs (NSAIDs), including aspirin and ibuprofen, blood pressure medications or heart medications.
- Over-use of nasal decongestant sprays (oxymetazoline) can cause rebound nasal congestion – “rhinitis medicamentosa”.
Complications from non-allergic rhinitis include:
- Nasal Polyps. These are benign growths that develop from the nasal and sinus lining. These can block sinus openings and even obstruct the nasal airway, making it difficult to breathe. An Otolaryngologist (Ear, Nose & Throat Doctor) should evaluate growth in the nose or sinuses.
- Chronic rhino-sinusitis (CRS). Prolonged swelling of the nasal and sinus lining can block the sinus openings, increasing the risk of developing sinusitis. Sinusitis lasting longer than 3 months is considered “chronic sinusitis”. It is nearly always associated with chronic rhinitis too, and the term chronic rhino-sinusitis has been adopted by experts.
- Ear Infections. Chronic swelling of the nasal lining tissues (mucosa) is often associated with inflammation and swelling of the Eustachian tube lining as well. Dysfunction of the eustachian tubes will result in middle ear infections – otitis media.
- Decreased quality of life. Chronic rhinitis, or CRS, have been shown to severely and negatively impact the quality of life – as much or even more than other chronic diseases that we think of as severely affecting the quality of life: diabetes or heart conditions.
What triggers Non-Allergic Rhinitis?
Non-allergic rhinitis, or vasomotor rhinitis, describes a group of other causes of rhinitis, with symptoms not caused by infection or allergy. Many people have recurrent or chronic nasal congestion, excess mucus production, itching, and other nasal symptoms similar to those of allergic rhinitis, but the disorder is not caused by the allergy.
Triggers of non-allergic rhinitis include:
- Irritants such as cigarette smoke, strong odors and fumes, including perfume, hair spray, other cosmetics, laundry detergents, cleaning solutions, pool chlorine, car exhaust and other air pollution.
- Spices used in cooking, alcoholic beverages (particularly beer and wine), aspirin and certain blood pressure medications.
- In some people, eating any foods (whether or not they are spicy) can cause nasal drainage because of a non-allergic nerve reflex. The medical term for this is gustatory rhinitis.
Some people are very sensitive to sudden changes in weather or temperature. Skiers often develop a runny nose, but in some people, any cold exposure may cause a runny nose. Others start sneezing when leaving a cold, air-conditioned room.
These factors are not allergens, do not induce the formation of allergic antibodies, and do not produce positive skin test reactions. Occasionally, one or two positive skin tests may be observed, but they do not match with the history and are not relevant or significant.
Treating non-allergic rhinitis
Treatment for non-allergic rhinitis often depends on the cause of the condition.
In some cases, such as when rhinitis is caused by a viral infection, treatment may not be necessary. This is because the infection responsible for the condition normally clears up within a week or two.
Avoiding triggers
If something specific seems to be triggering your symptoms, you may be advised to avoid possible triggers. For example, it may help to avoid exposure to smoky or polluted environments.
If your rhinitis is believed to be caused by a medication you’re taking, such as beta-blockers, your GP may be able to prescribe an alternative medication to see if it helps to reduce your symptoms. Don’t stop taking any prescribed medication unless advised to by a doctor.
Some cases of non-allergic rhinitis are caused by overusing nasal decongestant sprays. In these cases, the best treatment is to stop using these sprays. However, this can be difficult, particularly if you’ve been using them for some time.
Try not using the spray in your least congested nostril first. After seven days this nostril should open up, at which point you should try to stop using the spray in your other nostril.
It may also help to rinse your nose using a saltwater solution (see below) and take antihistamine tablets that cause drowsiness to reduce night-time congestion and help you sleep.
Some specialists try to gradually switch your spray from a decongestant (which is harmful in the long term) to a steroid spray (which generally can be used for longer periods).
Cleaning the nasal passages
In many cases of non-allergic rhinitis, rinsing your nasal passages with a saltwater solution can be helpful. This is known as nasal irrigation or nasal douching.
Rinsing your nasal passages helps wash away any excess mucus or irritants inside your nose, which can reduce inflammation and relieve your symptoms.
Nasal irrigation can be done using either a homemade solution or a solution made with sachets of ingredients bought from a pharmacy. Small syringes or pots (which often look like small horns or teapots) are also available to help flush the solution around the inside of your nose.
To make the solution at home, mix a teaspoon of salt and a teaspoon of bicarbonate of soda into a pint of boiling water that’s been left to cool to around body temperature (don’t attempt to rinse your nose while the water is still hot). To rinse your nose:
- standing over a sink, cup the palm of one hand and pour a small amount of the solution into it
- sniff the water into one nostril at a time – an alternative is to use a syringe to insert the solution into the nose
- repeat this until your nose feels comfortable (you may not need to use all of the solutions)
While you do this, some solution may pass into the throat through the back of the nose. Although the solution is harmless if swallowed, try to spit out as much of it as possible.
Nasal irrigation can be carried out several times a day and a fresh solution should be made each time.
Nasal sprays
Various types of nasal spray are available to help relieve the symptoms of non-allergic rhinitis. These include:
- Antihistamine nasal sprays – these help to relieve congestion and a runny nose by reducing inflammation
- Corticosteroid nasal sprays – like antihistamines, these work by reducing inflammation
- Anticholinergic nasal sprays – these reduce the amount of mucus your nose produces, which helps to relieve a runny nose
- Decongestant nasal sprays – these relieve congestion by reducing swelling of the blood vessels inside your nose
Many of these sprays can be bought over the counter in pharmacies without a prescription. Therefore, it’s important to check the leaflet that comes with them before use, because they’re not suitable for everyone.
Who gets Rhinitis?
Rhinitis is common. It can affect anyone of any age although it affects adults more commonly than children. It is becoming increasingly common in older people. Many people with persistent rhinitis say they have a persistent cold. However, colds are due to viral infections and normally only last a week or so. Persistent rhinitis is not due to an infection.
Allergic rhinitis (be it hay fever or persistent rhinitis) tends to run in families. You are also more likely to develop allergic rhinitis if you already have asthma or eczema. Equally, if you have allergic rhinitis, you are more likely to develop eczema or asthma. The conditions of asthma, eczema and allergic rhinitis are known together as atopic conditions or atopy. A tendency to atopy can run in families.
How do you know what kind of rhinitis you have?
Consult your physician. Sometimes several conditions can coexist in the same person. In a single individual, allergic rhinitis could be complicated by vasomotor rhinitis, septal deviation (curvature of the bone separating the two sides of the nose) or nasal polyps. Use of spray decongestants for chronic sinusitis, septal deviation or vasomotor rhinitis may cause rhinitis medicamentosa.
Any of these conditions will be made worse by catching a cold. Nasal symptoms caused by more than one problem can be difficult to treat, often requiring the cooperation of an allergist-immunologist and an otolaryngologist (ear, nose and throat specialist).
Tests and Diagnosis
Your doctor will perform a physical examination, take a medical history and possibly recommend one or both of the following tests:
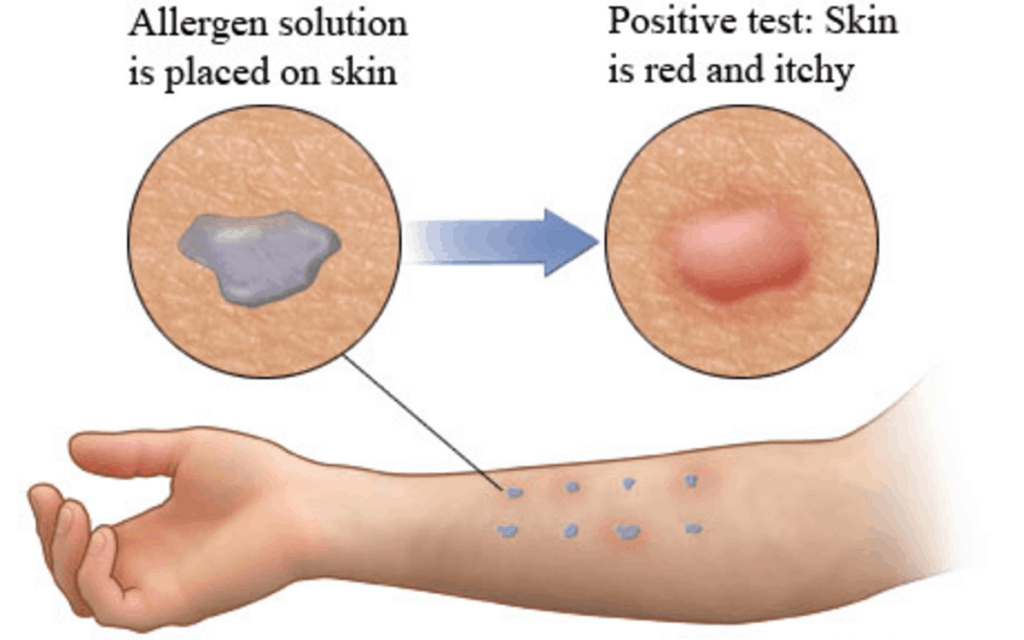
- Skin prick test. You’re watched for an allergic reaction after small amounts of material that can trigger allergies are pricked into the skin of your arm or upper back. If you’re allergic, you develop a raised bump (hive) at the site of that allergen. Allergy specialists usually are best equipped to perform allergy skin tests.
- Allergy blood test. A blood sample is sent to a lab to measure your immune system’s response to a specific allergen. Also called the radioallergosorbent test (RAST), this test measures the amount of allergy-causing antibodies in your bloodstream, known as immunoglobulin E (IgE) antibodies.
Rhinitis and NAET
Causes of allergic rhinitis can be tested by NTT (Nambudripad’s Testing Techniques) and treated very effectively with a non-invasive holistic approach known as NAET. (Source: NAET Official Website)
Most people suffering from Rhinitis feel better in warm, sunny weather because cold, damp weather patterns frequently cause the patient to feel chills. As a result, most of them require more bedding and warmer clothing.

Many patients with pollen allergies will also be allergic to certain foods, as well as to other inhalants and contactants (any substance that might induce an allergy by coming in contact with the skin or a mucous membrane). Other than pollen and grasses, the most common items found to cause hay fever are: sugar, carob, corn, wheat, beans, pineapple, tomato, banana, perfume, furniture, cats, dogs, feathers, kapok, dust, plastics, rubber, and leather.
It is extremely important that hay fever and rhinitis sufferers consult an appropriate allergist knowledgeable in NAET when their symptoms begin. These conditions have a tendency to become increasingly severe with each severe attack. Untreated patients are also likely to accumulate new allergens, as well as encounter increased sensitivity.
Rhinitis may also be caused by other substances including house dust, cigarette smoke, strong perfume, chemical sprays, household cleaning chemicals, occupational dusts (such as flour, silica, cement and metallic dusts, industrial dust), chalk powder, marker-inks, coloring crayons, newspaper, copying paper, recycled paper, newspaper-ink, house-paint, water and oil-based paints, crude oil, formaldehyde, cosmetic agents, soaps, perfumes, and other chemical agents.
Prompt treatment of these allergies greatly decreases the likelihood that a comparatively mild allergic manifestation, such as hay fever or allergic rhinitis, will develop into a more severe allergy, such as asthma.
How does it work?
By clearing all your environmental, heavy metal and food allergies from the protocol, we strengthen the immune system, improve digestion and absorption. This allows the body to get the necessary nutrients, which are essential for life. without causing any reactions.
One allergen is cleared per visit. Each individual has a different genetic makeup and health history so the number of sessions required varies from one individual to another. For some people, allergens are cleared immediately however, for others it may take many sessions to accomplish the desired results.
Some people might raise their eyebrows and ask, “Can you really eliminate my Rhinitis?” We answer with a resounding “YES!”
Evaluation may reveal energy interference in the lung, stomach, spleen, and large intestine meridians. Allergic rhinitis can be eliminated in most cases when the allergens are identified and desensitized.
NAET is Great!
I suffered from hay fever since the age of twelve, ever since I moved to Norwalk, California. Dr. Devi treated me for my allergy to yeast, pollens, grasses, flowers, perfumes, and mold. I have been totally symptom-free for the past 13 years.
Janna Gossen
La Mirada, CA
Connect with us through our Facebook page at www.facebook.com/NAETDubai or visit: www.naetdubai.com. You will find a wealth of information here along with an opportunity to speak confidentially through WhatsApp 056-639 0197 or Phone Call 04-420 1633.
You may also email us at admin@naetdubai.com