Allergy to Chemicals caused my Dermatitis
A 39-year-old woman developed asthma from the jewelry cleaning lotion she used in her trade. Similarly, a jeweler developed contact dermatitis from the sulfuric acid used as a cleaning agent, resulting in deep wounds on both hands and requiring constant glove use. These cases highlight how untreated or poorly managed skin conditions—such as contact dermatitis and atopic dermatitis—can worsen significantly over time. Seeking a permanent dermatitis cure is essential to prevent these conditions from progressing into more serious health issues like asthma or chronic infections.
If conditions such as eczema or dermatitis are merely suppressed with steroid creams, rather than addressed at the root, they can progress to more serious issues like asthma. That’s why many now seek a permanent dermatitis cure—one that eliminates the underlying cause rather than just masking symptoms.
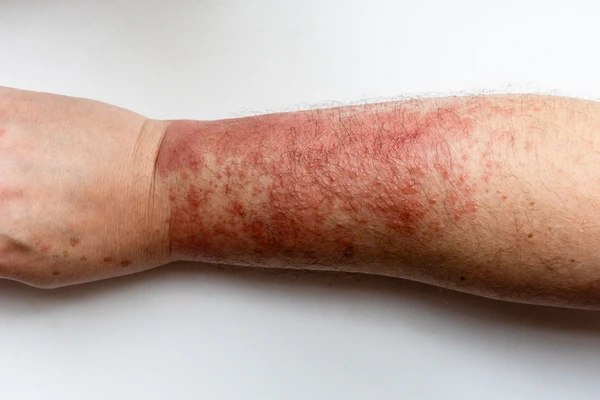
What is Dermatitis and How to Find a Permanent Cure?
Dermatitis is an inflammation of the skin. The word “dermatitis” is used to describe a number of different skin rashes that are caused by infections, allergies, and irritating substances.
Other inflammatory skin conditions like acne also have hidden causes rooted in immune response and internal health. Discover how we treat acne at the root.
Most Common Types of Dermatitis
1. Atopic Dermatitis
Atopic Dermatitis is a condition that causes itchy, inflamed skin. It typically affects areas like the insides of the elbows, backs of the knees, and the face, but in some cases, it can spread across most of the body. Atopic dermatitis belongs to a group of conditions known as atopic diseases, which also includes asthma and hay fever. People living in urban environments or low- humidity climates are at higher risk. While conventional treatments often manage symptoms temporarily, many are now searching for a permanent dermatitis cure that addresses the root cause and provides lasting relief.
Causes of Atopic Dermatitis & Paths to a Permanent Cure
Atopic dermatitis is caused by a skin reaction—similar to an allergy—that leads to ongoing swelling and redness. This often occurs because the skin lacks certain protective proteins, making it more sensitive to irritants.
The condition is most common in infants, starting as early as 2 to 6 months of age, though many outgrow it by early adulthood. People with atopic dermatitis frequently have asthma or seasonal allergies, and there is often a family history of conditions like asthma, hay fever, or eczema. They also tend to test positive on allergy skin tests. This combination of genetic and immune sensitivity can trigger related skin issues like acne. That’s why many are now turning to holistic approaches that offer a permanent dermatitis cure, addressing the root cause rather than just the surface symptoms.
The following can make atopic dermatitis symptoms worse:
- Allergies to pollen, mould, dust mites, or animals
- Cold and dry air in the winter
- Colds or the flu
- Contact with irritants and chemicals
- Contact with rough materials, such as wool
- Dry skin
- Emotional stress
- Drying out of the skin from taking frequent baths or showers and swimming very often
- Getting too hot or too cold, as well as sudden changes in temperature
- Perfumes or dyes added to skin lotions or soaps
What are the symptoms of atopic dermatitis?
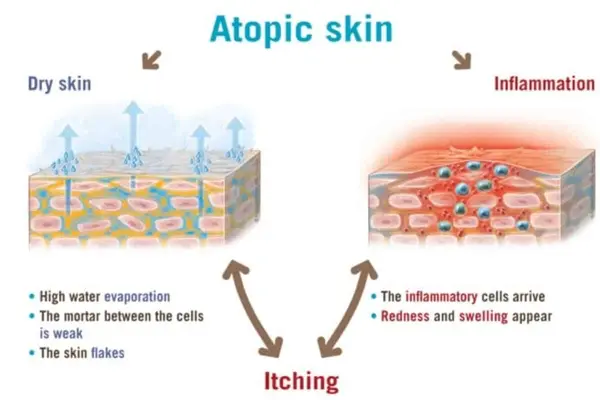
The primary symptom of atopic dermatitis is dry, itchy skin that often turns into a red rash. During a flare, the condition worsens into intensely itchy, inflamed patches. Many physical and internal factors can trigger these flare-ups, with inflammation increasing blood flow and the urge to itch.
Eczema flares contribute to the relentless itch-scratch cycle, which is both physically and psychologically difficult to break. While scratching may bring temporary relief, it often leads to more inflammation and even skin infections.
Similarly, chronic acne presents with red, irritated lesions. For those battling eczema, seeking a permanent dermatitis cure can help break this painful cycle and bring permanentdermatitis cure.
Atopic dermatitis presents different symptoms depending on a person’s age.
Symptoms in infants can include:
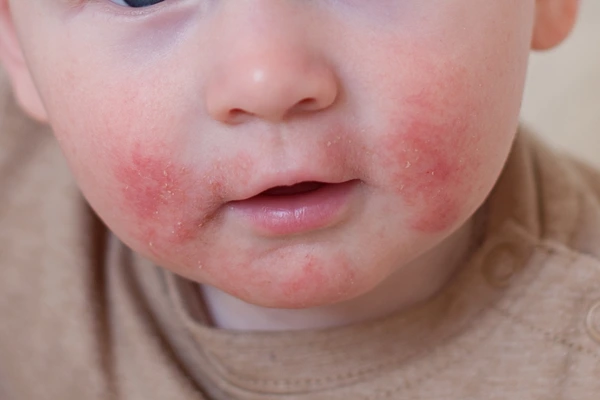
- dry, itchy, scaly skin
- a rash on the scalp or cheeks
- a rash that may bubble and weep clear fluid
Infants with these symptoms may have trouble sleeping due to itchy skin. Infants with atopic dermatitis may also develop skin infections from scratching.
Symptoms in children can include:
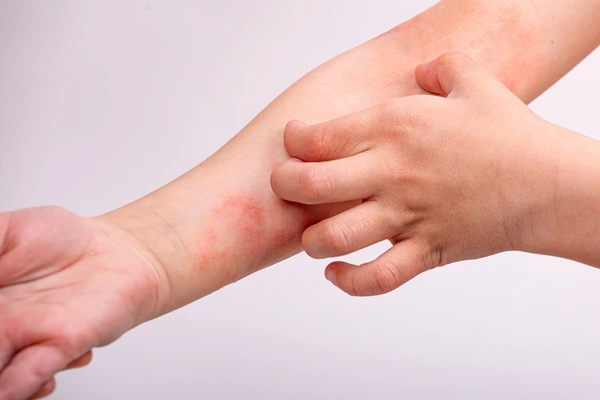
- a rash in the creases of the elbows, knees, or both
- scaly patches of skin at the site of the rash
- lightened or darkened skin spots
- thick, leathery skin
- extremely dry and scaly skin
- rashes on the neck and face, especially around the eyes
Symptoms in adults can include:
Adults who had atopic dermatitis as children may have discoloured skin that is easily irritated.
Who Gets Atopic Dermatitis?
Atopic dermatitis is most common in babies and children, though it can affect people of all ages. Those living in cities and dry climates may be more prone to developing this condition.
In some cases, children outgrow atopic dermatitis as they get older, but their skin often remains dry and easily irritated. For others, the condition continues into adulthood.
While it isn’t contagious and can’t be passed from person to person, the persistent nature of the symptoms leads many to seek a permanent dermatitis cure that offers permanentt cure instead of temporary fixes.
Dermatitis Treatments: From Medication to Permanent Cure
Medications
- Creams that control itching and inflammation.Your doctor may prescribe corticosteroid creams or ointments to reduce symptoms. However, long-term use can lead to side effects like thinning skin, stretch marks, infections, or discolouration. While these creams offer short-term relief, they do not provide a permanent dermatitis cure.
- Creams that help repair the skin.Calcineurin inhibitors such as tacrolimus (Protopic) and pimecrolimus (Elidel) support skin healing by regulating immune activity. These prescription creams are typically used when other treatments fail. Since they carry potential side effects, they are not a long-term solution for those seeking a permanent dermatitis cure.
- Drugs to fight infection.If scratching causes cracked skin or bacterial infection, your doctor may prescribe antibiotics either short term or longer term to prevent recurrence. While helpful in managing complications, they are not part of a permanent dermatitis cure, which focuses on eliminating root triggers.
- Oral anti-itch drugs.Antihistamines like diphenhydramine (Benadryl) may ease nighttime itching by promoting sleep. Though they relieve discomfort, they do not address the cause and are not a permanent dermatitis cure.
- Oral or injected drugs that control inflammation.Corticosteroids such as prednisone are powerful in severe cases but carry serious side effects when used long term. These are temporary solutions, making it important for patients to explore options aimed at a permanent dermatitis cure for long-lasting relief.
Therapies That Support a Permanent Dermatitis Cure
- Wet dressings.An effective, intensive treatment for severe atopic dermatitis involves wrapping the affected area with topical corticosteroids and wet bandages. It can reduce symptoms within hours or days and is sometimes performed in hospitals due to the need for nursing supervision. While this method offers fast relief, it is not a long-term solution. For lasting results, many patients look for a permanent dermatitis cure that addresses the condition from its root.
- Light therapy. The simplest form of light therapy (phototherapy) involves exposing your skin to controlled amounts of natural sunlight. Other types use UVA or narrowband UVB light, sometimes in combination with medications. While phototherapy may provide symptom relief, prolonged use carries risks like premature skin aging and skin cancer. Because of these limitations, many prefer safer, natural alternatives that aim for a permanent dermatitis cure without harmful side effects.
- Treatment for stress.Counselling may help children and young adults who are extremely embarrassed or frustrated by their skin condition. Emotional wellbeing is important, but to truly resolve the issue, stress support should be combined with an approach that seeks a permanent dermatitis cure.
- Relaxation, behaviour modification or biofeedback.These approaches may help you with habitual scratching. Managing the urge to scratch is important, but combining it with a comprehensive treatment that targets the underlying triggers is key to achieving a permanent dermatitis cure.
2. Contact Dermatitis

When your skin comes into contact with the substance in the environment that you are allergic to, it may react by causing your skin to itch and become red. This is called contact dermatitis.
Allergic Reaction Triggers
If it’s an allergy, your immune system is involved. After you touch something, it mistakenly believes your body is under attack and responds by producing antibodies. This triggers a chain reaction that releases chemicals like histamine, which leads to an allergic response—often in the form of an itchy rash known as allergic contact dermatitis. While creams may offer short-term relief, addressing the immune system’s overreaction is essential for a permanent dermatitis cure.
Common triggers for contact dermatitis are:
- Poison ivy, poison oak, and poison sumac
- Hair dyes or straighteners
- Jewellery
- Nickel, a metal found in jewellery and belt buckles
- Leather (specifically, chemicals used in tanning leather)
- Latex rubber
- Citrus fruit, especially the peel
- Fragrances in soaps, shampoos, lotions, perfumes, and cosmetics
- Some medications you put on your skin
Usually, you won’t get a rash the first time your skin touches something you’re allergic to. That initial contact sensitizes your skin, making it more likely to react the next time. If you develop a rash on first contact, it’s likely you’ve encountered the trigger before without realizing it. Identifying and addressing these hidden triggers is essential when seeking a permanent dermatitis cure that goes beyond just treating surface symptoms.
Symptoms of contact dermatitis include:
- Red, irritated skin
- Itching
- Swelling
- Bumps or blisters, sometimes filled with clear fluid
- Hot or tender skin
These symptoms can range from mild to severe, and they can appear anywhere from a few hours to 10 days after coming into contact with the irritant or allergen. A contact dermatitis rash cannot be spread to anyone else.
If you’ve come into contact with a potential allergen or irritant, immediately wash the affected area with soap and water.
Treatment for Contact Dermatitis
Treatment is the same for both types of contact dermatitis.
Avoid what is causing your rash. If avoiding the cause will be difficult, ask your dermatologist for help.
For example, if you are allergic to latex but must wear exam gloves, your dermatologist can recommend an alternative material. Similarly, if you need to work outdoors where poison ivy is present, they may suggest a protective barrier cream and suitable clothing. While treating the rash is important, avoiding the trigger is key. Once the cause is identified and avoided, the rash should clear. To further relieve symptoms, your dermatologist may recommend various treatments. However, for long-term relief, many patients look beyond temporary fixes and seek a permanent dermatitis cure that addresses the root cause.
- Mild reaction: Antihistamine pills, moisturizer, and a corticosteroid that you can apply to your skin. Most patients apply for medicine twice a day for 1 week and once a day for 1 to 2 weeks. Oatmeal baths can relieve discomfort.
- In cases of severe reaction, if you experience significant swelling, facial puffiness, or a rash that spreads over much of your body, you may need a stronger medication. In such situations, your dermatologist may prescribe prednisone. It’s important, however, to take this medication exactly as directed to prevent another flare-up. Additionally, wet dressings can help soothe skin with heavy oozing and crusting. If your dermatologist recommends wet dressings, you’ll also receive clear instructions on how to prepare and apply them at home.
3. Managing Neurodermatitis: Is a Permanent Dermatitis Cure Possible?
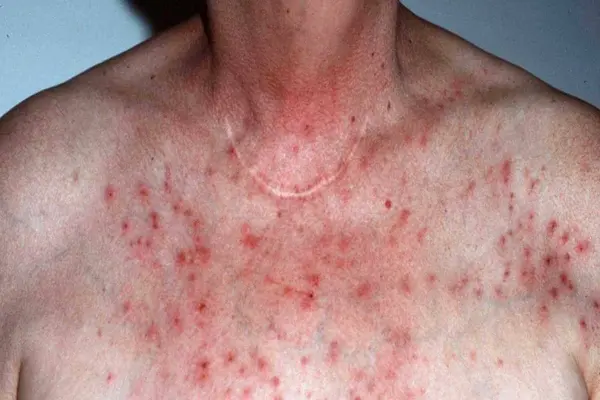
Neurodermatitis is a skin condition that starts with a patch of itchy skin. Scratching makes it even itchier, creating an itch-scratch cycle that causes the affected skin to become thick and leathery. You may develop several itchy spots, typically on the neck, wrist, forearm, thigh, or ankle.
Neurodermatitis — also known as lichen simplex chronicus — is not life-threatening or contagious. However, the intense and recurring itching can severely affect sleep, sexual function, and overall quality of life. That’s why many people now seek a permanent dermatitis cure to break the cycle and restore comfort without relying on temporary relief.
What are the causes of Neurodermatitis?
Scientists have yet to find the exact cause of this problem, however, there are a number of trigger points that have been associated with the lichen simplex chronicus condition, this includes:
- Clothing is worn tightly and made of synthetic fabric or wool
- Dry skin
- These triggers are less frequent but could result in a neurodermatitis attack
- Exhaust from traffic (long-term exposure)
- Exposure to allergens and skin irritants (i.e.hair sprays or dyes)
- Heat exposure
- Insect Bites
- Prolonged periods of intense stress or emotional trauma
- Lack of adequate blood flow or poor circulation
- Keloid Scars
Symptoms of Neurodermatitis
Signs and symptoms of neurodermatitis include:
- An itchy skin patch or patches
- The leathery or scaly texture on the affected areas
- A raised, rough patch or patches that are red or darker than the rest of your skin
The condition involves areas that can be reached for scratching — the head, neck, wrist, forearm, ankle, vulva, scrotum or anus. The itchiness, which can be intense, may come and go or be nonstop. You may scratch out of habit and while sleeping.
Neurodermatitis Treatment
Because this condition is accompanied by excessive itching and scratching, the objective of treatment is to eliminate this reaction. The following are known treatments that have been prescribed by a physician:
1. Topical corticosteroid to reduce inflammation and alleviate the itch.
2. Topical antibiotics can fight infection in the event a breakage of the skin has occurred from the scratching.
3. An oral antibiotic is a more powerful medication to eliminate any secondary infection.
4. Topical keratolytic is a preparation containing urea, salicylic acid, or lactic acid that can help in the reduction of thick skin.
In severe cases, doctors have prescribed a sedative or tranquillizer. This is used in cases of severe anxiety to induce sleep.
4. Can Stasis Dermatitis Be Healed? Exploring a Permanent Dermatitis Cure
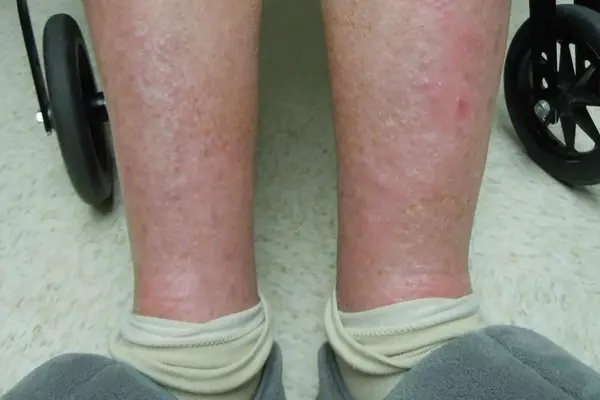
Stasis dermatitis is a skin condition that develops in people with poor circulation. It typically occurs in the lower legs. In serious cases, stasis dermatitis can progress into ulcers.
Common Causes of Stasis Dermatitis
Poor circulation causes stasis dermatitis. Typically, poor circulation is the result of a chronic, or long-term, the condition called venous insufficiency. Venous insufficiency occurs when your veins have trouble sending blood to your heart. There are one-way valves inside your leg veins that keep your blood flowing in the right direction, which is toward your heart.
In people with venous insufficiency, these valves become weak. This allows blood to flow back toward the feet and pool in your legs instead of continuing to flow toward your heart. This pooling of blood is what causes stasis dermatitis.
Varicose veins and congestive heart failure are also known causes of leg swelling and stasis dermatitis.
Most of the conditions that cause stasis dermatitis usually develop in people as they get older. However, there are also several causes that are unrelated to age, including:
- surgery, such as using a leg vein for bypass surgery
- deep vein thrombosis in your leg
- traumatic injury to your lower legs
Stasis Dermatitis Symptoms
Stasis Dermatitis affects the legs of a person. Naturally, the symptoms of this disease are mainly visible in the legs of the sufferer. But it can also affect other body parts like the arms if they suffer from poor blood circulation. The symptoms include :
- The appearance of red rashes
- Itching in the affected area
- Accumulation of fluids under the weakened skin region
- Darkening or thickening of the skin in the ankles or legs
- Development of ulcers and sores in the weak skin area
- Pain in the legs
- Cracks in the affected region of the skin
- Thickened skin in the affected leg region
- Formation of lesions in the legs
Stasis Dermatitis Treatment
There are several things you can do at home to treat stasis dermatitis. You should:
- avoid standing and sitting for long periods of time
- prop up your feet when sitting
- wear compression stockings
- wear loose-fitting clothing to avoid irritating your skin
Ask your doctor about the types of skin creams and ointments you can use. You should avoid using the following products:
- lanolin
- calamine and other lotions that dry your skin
- topical antibiotic ointments such a neomycin
- benzocaine and other numbing medications
5. Seborrheic Dermatitis: Root Causes and Permanent Cure Options
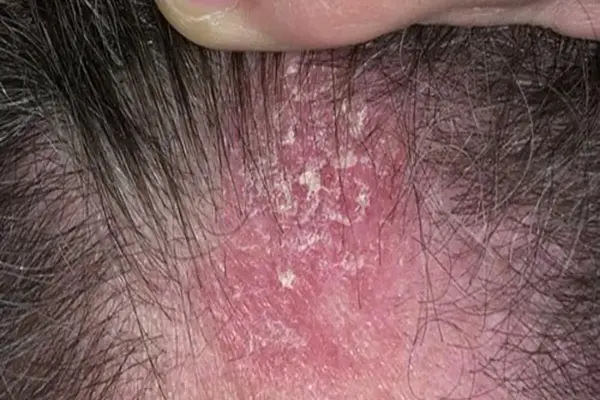
Seborrheic dermatitis, also known as seborrheic eczema or simply as seborrhea, is a chronic, relapsing and usually mild dermatitis. In infants, seborrheic dermatitis is called cradle cap. Dandruff is a type of seborrheic dermatitis where inflammation is not present. Seborrheic dermatitis is a skin disorder affecting the scalp, face, and torso.
Causes of Seborrheic Dermatitis
Although the exact cause is unknown, several contributing factors may play a role in the development of seborrheic dermatitis. For instance, abnormalities in the oil glands and hair follicles, as well as the presence of a yeast fungus with bacteria growing in the sebum, may be involved. Additionally, the production of certain hormones, combined with stress, seasonal changes (outbreaks often worsen in winter), and fatigue, can all contribute to flare-ups.
Seborrheic Dermatitis Symptoms
Seborrheic dermatitis symptoms include:
- Skin flakes (dandruff) on your scalp, hair, eyebrows, beard or moustache
- Patches of greasy skin covered with flaky white or yellow scales or crust on the scalp, ears, face, chest, armpits, scrotum or other parts of the body
- Red skin
- Redness or crusting of the eyelids (blepharitis)
- Possibly itching or stinging
Treatment for seborrheic dermatitis
Treatment of hair-bearing areas, like the scalp, often includes the use of a shampoo that may contain one or more of the following ingredients:
- Tar
- Antifungal antibiotic
- Zinc pyrithione
- Selenium sulfide
In addition, the application of a topical steroid lotion or solution of weak to moderate potency is effective such as desonide (Desonate, DesOwen, LoKara, Verdeso), betamethasone valerate (Valisone), hydrocortisone, and 0.025% triamcinolone (Aristocort, Aristocort HP, Kenalog, Triderm).
For non-hair-bearing areas, the application of a weak to moderately potent topical steroid or topical antifungal cream is frequently effective. The use of tacrolimus (Protopic) or pimecrolimus (Elidel) ointments can be effective but is quite an expensive alternative.
It needs to be stressed that since this condition is incurable but easily controllable; if the disease is active and the treatment is stopped, one should expect seborrheic dermatitis to recur. One should also use effective medications just enough to control the symptoms. Excessive treatment of apparently normal skin is economically wasteful as well as potentially risky.
How We Treat Dermatitis for a Permanent Cure
With us, we get to the root of the problem, identifying and eliminating the allergen that is causing the recurring symptoms.
We offer the prospect of relief to those who suffer from addiction and allergies by reprogramming the brain to perfect health. Just like rebooting a computer, we can reboot our nervous system to overcome the adverse reactions of brain and body.
To fully understand what we do, one needs to know some traditional healing principles. We take concepts from acupuncture and traditional medicine and have developed a technique that can eliminate the reaction from the root.
Addictions can definitely cause illness. Continuous contact with an allergen produces toxins in the body and causes blockages in the meridians. If these blockages are not cleared, reactions to the allergens often produce symptoms that mimic other diseases.

By clearing all your environmental, heavy metal and food allergies from the protocol, we strengthen the immune system, improve digestion and absorption. This allows the body to get the necessary nutrients, which are essential for life. without causing any reactions.
This method has also helped many clients struggling with persistent acne.
One allergen is cleared per visit. Each individual has a different genetic makeup and health history so the number of sessions required varies from one individual to another. For some people, allergens are cleared immediately however, for others it may take many sessions to accomplish the desired results.
Some people might raise their eyebrows and ask, “Can you really eliminate my Dermatitis?” We answer with a resounding “YES!”
46 YEARS OF DERMATITIS CLEARED BY NAET
A man who suffered his first attack of dermatitis at the age of five did not consult an allergist until he was 46. By then, atopic dermatitis had spread across his entire body, becoming chronic and distorting his skin so severely that the resulting scars may be permanent. Over four decades, his eczema worsened and was further complicated by hay fever and asthma. Unlike typical childhood dermatitis that fades during puberty, his symptoms persisted and intensified with age.
When he finally sought help, allergy testing revealed sensitivities to multiple foods, pollens, inhalants, and even medications he had been using. After trying conventional treatments with no success, he visited our office. Through targeted desensitization to foods, fabrics, and environmental triggers, he experienced marked improvement. However, because the condition had been left untreated for so long, a full recovery will take years—even though he is now symptom-free. This case highlights the importance of early intervention and the consequences of delaying a permanent dermatitis cure.
Poison ivy and poison oak are classic examples of allergens that can trigger contact dermatitis. These reactions are true allergies, as not everyone is affected, and some may require only a single exposure to become sensitized. Identifying such triggers early is essential for those seeking a permanent dermatitis cure and long-term relief.
Connect with us through our Facebook page at www.facebook.com/NAETDubai or visit: www.naetdubai.com. You will find a wealth of information here along with an opportunity to speak confidentially through WhatsApp 056-639 0197 or Phone Call 04-420 1633.
You may also email us at admin@naetdubai.com

4 Responses
Thank you for your comment ???? . Please don’t forget to subscribe to our blog and you will receive mails once we published new blogs. Feel free to contact us if you need any further information. Cheers!
Thank you for your comment.Please dont forget to subscribe to our blog and feel free to contact us for any further details.
Thank you so much for your comment. Please don’t forget to subscribe to our blogs. Feel free to contact us if you need any further information.
Not only the articles are excellent but NAET is. It healed my histamin. fructose, apple, eggs, pet hair allergy. It changed my life completely. Give it a try … it is worth to do it. Don’t suffer for the next years.